Spinal Infection – Causes, Symptoms, And Recovery
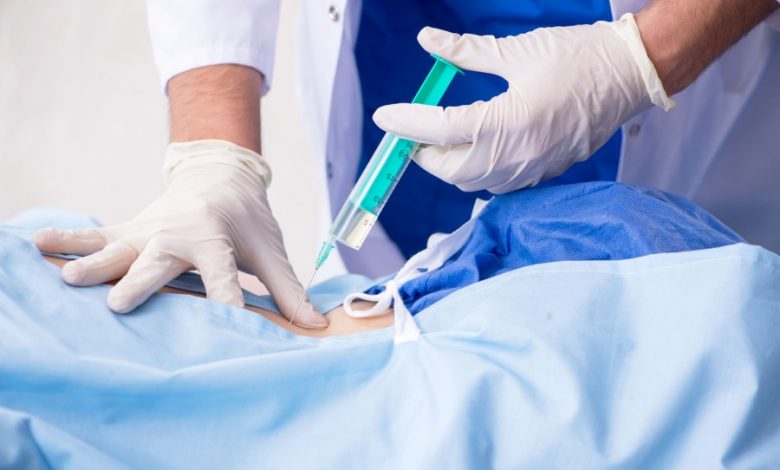
Spinal infections are uncommon but potentially fatal, so you should seek medical attention as soon as possible if you’re enduring back pain, fever, and other symptoms causing discomfort.
Please continue reading to learn more about spinal infections, the various kinds of spinal illnesses, how to recognize them, and how to cure them. Each type of spine infection has its own set of causal factors, clinical signs, and treatment options.
What are Spinal Infections?
Spinal infections are microbial or fungal infections that affect the vertebrae or spinal column. Depending on the type of spinal infection, they can cause many health problems.
For example, if your illness affects the room between both the vertebral bodies in your backbone, you may experience trouble urinating, losing weight, pyrexia, and severe back pain. Discitis is a representation of such an infectious disease.
If you assume you have a spinal infection, see your doctor and get a medical evaluation as soon as possible. Or else the infection could cause permanent damage to your spine and surrounding areas.
Types of Spinal Infections
The following are examples of spinal infections:
-
Vertebral Osteomyelitis:
These infections most commonly affect the lower back and can induce shoulder or knee pain, pyrexia, loss of weight, muscle cramps, and difficulty moving or using your hands.
-
Discitis spinal infection:
This unusual infection is caused independently or as a result of surgery. Symptoms include back pain, emitting pain throughout the body, and fevers and shivers.
-
Spinal Epidural Abscess:
These spinal infections are most frequently found in the lower spine, and can cause frailty, skin boils, backache, shoulder or leg pain, vertebral soreness, and intestinal, urinary system, and abdomen issues.
-
Spinal Subdural Empyema:
It is a very unusual spinal infection that usually results from some other infection. It can result in a fever as well as arm or leg pain.
-
Meningitis:
This infestation, which causes inflammation in the tissues surrounding the brain and spine, can be dispersed quickly and cause serious medical problems if not handled correctly.
-
Spinal Cord Abscess:
Spinal cord infection, which occurs internally in the vertebrae, is extremely rare. It can result in fever, back problems, and decreased spine activity.
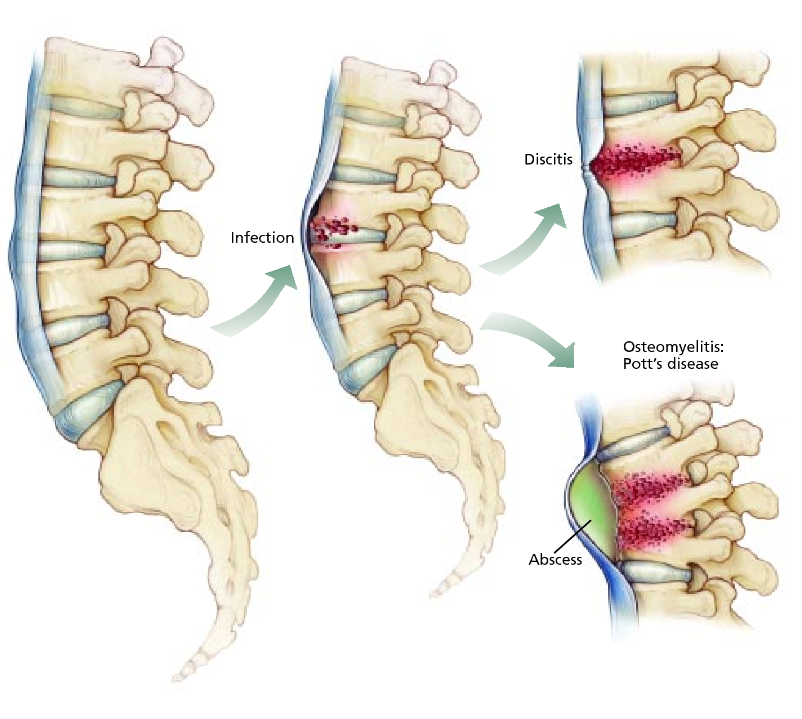
What Are The Causes of Spinal Infections?
The causes depend on the type of spinal infection one person is facing. We will separately discuss the causes associated with different infections:
-
Cause of Osteomyelitis:
Osteomyelitis is a spinal infection caused by bacteria, pathogens, or fungi extending into your spine. There are several ways they can get into your spinal column, such as:
- Surgery. Vertebral metalwork, for example, can cause infections.
- Infection propagating from nearby tissues
- Infections of the plasma
-
Cause of Discitis spinal infection:
This is an infectious disease that can occur due to surgical procedures or on its own. Staphylococcus aureus is the most frequent cause, and other bacteria such as Streptococcus can induce it.
Discitis can occur due to a bladder infection or pneumonia extending throughout your body via your blood system.
-
Cause of Meningitis:
It can be contagious or noncontagious. This means that it can be induced by drugs, abnormalities, pathogens, and other living things. When a virus causes meningitis, the brain tissue is unaffected. If you suffer from bacterial meningitis, your brain may be influenced.
-
Cause of Spinal Epidural Abscess:
This spinal infection is generally caused by a bacterium known as Staphylococcus aureus. It could also be caused by a fungus or some other microbe circling in your bloodstream. Often, healthcare professionals cannot pinpoint the source of an infectious disease.
-
Cause of Spinal Subdural Empyema:
Even though staphylococcal bacteremia is the most common cause of spinal subdural empyema, it can also be caused by a spinal epidural abscess, continual dermal sinus, osteomyelitis, spinal surgery, epidural anesthesia, or acupuncture.
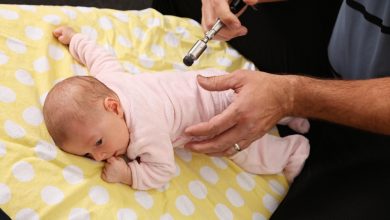
Interesting Read: Here’s all you need to know about chiropractic care for babies
What Are The Symptoms of Spinal Infections?
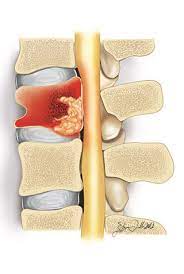 The symptoms of a vertebral infection usually appear gradually. For instance, it could take you a week to realize you’re getting a cold.
The symptoms of a vertebral infection usually appear gradually. For instance, it could take you a week to realize you’re getting a cold.
The following are clear common indicators of a spinal infection:
- Neck tightness or back pain
- Fever, shivers, or upset stomach
- Sweating at night
- Back pain that worsens at night or does not go away with rest
- A reduction in movement or range of motion
- Rashes or warmth at surgery incision sites or on the surface of the skin
- Surgical scars that leak pus or do not heal.
Treatments For Spinal Infections:
There are two possible ways to treat spinal infections. It all depends on the severity of your infections and how long it has been that you have been suffering from the infection.
-
Treatment Without Surgery:
Spinal infections frequently necessitate lengthy intravenous antibiotics or antifungal rehab, resulting in the patient being hospitalized for an extended period. Immobilization may be suggested when there is a substantial ache or the possibility of spine destabilization. If the patient is neurologically and is stable, antibiotic treatment should be started once the pathogen causing the disease has been recognized.
Antimicrobial therapy is typically administered to patients for at least six to eight weeks. The medicine is decided individually based on the person’s particular circumstances, such as age.
Also Read: Can chiropractors write prescriptions?
-
Surgical Treatment of spinal infection:
When patients have limited or no nerve damage and the mortality rates of invasive surgery are strong, nonsurgical spinal infection treatment is recommended first. Nevertheless, surgery may be suggested if any of the following conditions exist:
- Spinal destabilization is caused by substantial tissue destruction.
- Deficiencies in neurological function
- Sepsis with diagnostic toxicity induced by a non-responsive abscess to antibiotics
- Failure of needle biopsy to acquire necessary cultures
- Intravenous medications alone were ineffective in eradicating the infection.
The stated objectives of spinal infection surgery are as follows:
- Disinfect the infected area and clean it.
- Allow adequate blood circulation to the affected tissues to aid in recovery.
- Rebuild spinal consistency by fusing the unsteady spine with equipment.
Spinal Infection Recovery Period:
The recovery period depends on the type of treatment you have opted for. In the case of nonsurgical treatments, doctors will give you the medication and antibiotics for 8 weeks. Oral antibiotics may be required for a few months. To assist manage symptoms, pain relievers and spinal bracing could be used. You may also be asked to join the rehab for therapy as it is proven to help gather positive results.
In the case of spinal surgery (decompression), the recovery time is 4 to 6 weeks. The doctors will monitor you to look for any possible defect or slow recovery. The spine will take some time to get back in place, and many instructions will be given to you for a speedy recovery. After the surgery, there is a chance that your back will feel sore, and you will be given some support for the infection to heal correctly.
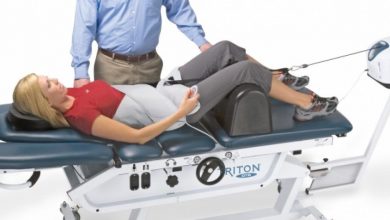
Interesting read: a complete guide to spinal decompression therapy
Final Thoughts
It is advised to get yourself checked as soon as possible if you are feeling fever, back pain, and other symptoms. A proper procedure can be followed in spinal infection to ensure that the problem does not get worse. Timely checkups and diagnoses can help you return to your everyday life. You should make sure to follow all the instructions given by the doctor to ensure a healthy recovery, as the infection can be turned into something that will complicate your life.